Why Is There Blood In My Stool
Blood in the stool is the result of bleeding in your gastrointestinal tract. The GI tract includes organs like the stomach, small intestine, and large intestine .
Seeing blood in your stool can be alarming. You may have heard blood in your stool can be a sign of cancer, but more often, bleeding is a symptom of a less serious condition.
Many conditions can cause it, including a bad case of diarrhea or constipation.
Symptoms of an emergency
Seek emergency attention if youre bleeding a lot. Also see a doctor if youre experiencing dizziness, weakness, and confusion alongside bleeding.
There are multiple causes of blood in the stool.
How Does Blood In The Stools Appear
According to the Canadian Institute of Intestinal Research, most people with UC experience varying levels of hematochezia, which refers to blood in the stools. The blood will usually be clearly visible in the stool â which has a semi-solid consistency â or on the surface. The blood color can range from bright red to maroon, with or without blood clots. This symptom often accompanies lower abdominal pain and the urgent need to defecate.
Blood from the rectum and large intestine is usually bright red. If blood is a darker color, it may be coming from higher up the gastrointestinal tract.
People with UC may have slow, steady bleeding when they do not have a bowel movement. They may also experience bloody diarrhea and constipation.
Some individuals with severe UC may notice blood in their stools more than 10 times a day.
People with UC will also usually have mucus in the stools but may not be able to see it. The mucus helps protect the inner lining of the intestines, as well as helping with bowel movements.
According to the Crohnâs and Colitis Foundation, people need immediate medical attention if they experience rectal bleeding with blood clots in stools.
What Side Effects Of Ibd Can Cause Malnutrition
There are several reasons why people with IBD may be at risk for malnutrition. The following list includes some side effects that contribute to malnutrition.
- Inadequate food/fluid intake may by caused by nausea, abdominal pain, loss of appetite or altered taste sensation
- Increased losses â intestinal inflammation during acute flares results in increased protein losses, losses from fistula fluids, diarrhea and bleeding
- Increased nutritional needs â inflammation or infection increases metabolic requirements
- Malabsorption with Crohns disease may be caused by severe intestinal inflammation, resection of small intestine and medications, such as prednisone and sulfasalazine
Also Check: Does Witch Hazel Shrink Hemorrhoids
What Is The Treatment For Rectal Bleeding From Crohn’s Or Uc
The treatment for rectal bleeding depends on the cause. When it is a symptom of IBD, treating the IBD is often an effective way to stop the bleeding.9
Similarly, bleeding due to complications from IBD is managed by treating the complication. For fissures, the first step is trying to let it heal on its own. If the fissure does not heal, medications and surgery are used. Anal fistulas also are treated with a combination of medication and surgery.
Killing Off The Bad Bugs

To get rid of disease-causing bacteria, viruses, yeast, mycobacteria and parasites in your gut, use Jinis Wild Oregano Oil Protocol . If you have a mycobacterial infection, you will need to cycle on and off this wild oregano oil protocol for 2 to 3 years to get rid of all the mycobacteria as they have an inactive/active lifecycle.
People generally start with Jinis Wild Oregano Oil Protocol and then after completing the first round of treatment, move to high dose, therapeutic probiotic supplementation. Remember, they have already begun probiotic supplementation with my Wild Oregano Oil Protocol, so their system doesnt usually have much difficulty making the change to high dose probiotics.
You May Like: What Foods To Eat When You Have An Ulcer
You May Like: What Is Used For Hemorrhoids
What Should I Ask My Doctor
If you have ulcerative colitis, you may want to ask your healthcare provider:
- How much of my large intestine is affected?
- What risks or side effects can I expect from the medication?
- Should I change my diet?
- Will ulcerative colitis affect my ability to get pregnant?
- What can I do at home to manage my symptoms?
- What are my surgical options?
Why Do You Get Anal Fissures And Hemorrhoids With Crohns Disease
Usually, you get anal fissures because youâre constipated: When youâre plugged up, a particularly large or hard BM can tear the lining of your butt canal. It can also be caused by too-tight anal sphincters . But with Crohnâs disease, there are some key differences:
- Your anal fissures are most likely due to the chronic inflammation of the lining of your GI tract.
- Youâre likely to have several anal fissures, rather than just one.
- Your fissures usually run down the sides of your butt, rather than the middle.
- You may also have skin tags in your butt canal that can be mistaken for hemorrhoids.
Hemorrhoids arenât as common as fissures if you have Crohnâs disease. If you do develop hemorrhoids, itâs thought that theyâre due not to the inflammation associated with Crohnâs, but to diarrhea or constipation related to it, which can put extra pressure on butt veins.
Read Also: How To Make Your Hemorrhoids Go Away
Identifying And Healing Emotional Causes Of Colitis
Over 60% of your bodys neurotransmitters are not in your brain, but in your gut! . There is now an entire field dedicated to this emerging knowledge about the interrelation of the mind, emotions and the digestive system, called neurogastroenterology.
This is not airy-fairy stuff this is hard science. Consider blushing a purely emotional event that instantly produces a marked physical reaction. Thats just one example of how the mind/emotions and body are inextricably linked. If you dont heal the psychological and emotional causes of colitis, then you will not have long-term vibrant health. Its really that simple.
In my experience, the most effective mind/body therapies to treat colitis and other colon and bowel disorders are , hypnotherapy and craniosacral therapy . You need to work with a skilled therapist, at least initially, to really see good results. And its best if you can use a therapist who is experienced with chronic illness like ulcerative colitis which is more complex than regular illness.
What Treatments Heal Rectal Ulcers Without Surgery
To relieve symptoms of a rectal ulcer and help it heal, you should:
- Drink plenty of water: Dehydration can make stool hard, dry and more difficult to pass.
- Eat a healthy diet: Fiber-rich foods can relieve constipation. Fiber softens stool and helps it pass through your intestines faster.
- Avoid straining: Straining or pushing too hard when defecating can cause rectal ulcers. Your doctor or physical therapist can show you how to control the muscles in your anus so you can have a bowel movement without damaging your anus or rectum.
- Ask your doctor about laxatives: Your doctor may recommend taking a stool softener or laxative. These medications can relieve constipation by making your stool easier to pass. Talk to your doctor about which laxative you should take and how long you should take it.
- Try a topical medication: A corticosteroid cream or suppository can reduce inflammation, relieve pain and help the ulcers heal. Talk to your doctor about how to use this medication.
- Take antibiotics: If an STD or STI is causing rectal ulcers, your doctor will prescribe medicine to treat the infection.
If you have an inflammatory bowel disease such as ulcerative colitis, your doctor will recommend a treatment plan. Your plan may include a combination of prescription anti-inflammatory drugs, immunosuppressant drugs and dietary changes.
Recommended Reading: Best Relief From Hemorrhoids Pain
What Supplements Should You Take For Crohns Disease Vs Ulcerative Colitis
Crohns disease nutritional diet deficiencies
- Your need for vitamin and mineral supplements depends on several factors, your diet, which parts of your digestive tract are affected, and whether you have had surgery on your small intestine.
- The most common vitamin deficiencies are
- vitamins D and B-12.
Ulcerative colitis nutritional deficiencies
As with Crohns disease, nutrition is important if you have ulcerative colitis because symptoms of diarrhea and bleeding can lead to dehydration, electrolyte imbalance, and loss of nutrients. It may be necessary to take nutritional supplements if your symptoms do not allow you to eat a nutritionally balanced diet. Talk to your health-care professional about what supplements to take.
Treatment For Colorectal Cancer
Talk with your doctor if you believe you have colorectal cancer. They can help determine a diagnosis, what stage the cancer is in if you do have cancer, and the right treatment for you. The earlier you get treatment, the better your outcome.
Diagnosis is first made with a biopsy, usually with colonoscopy or flexible sigmoidoscopy depending on the location of the tumor. Afterward, imaging is done so your doctor can see the extent of the disease before they make a plan for surgery, chemotherapy or radiation.
Recommended Reading: When Should I Go To Doctor For Hemorrhoids
What Is Ulcerative Colitis
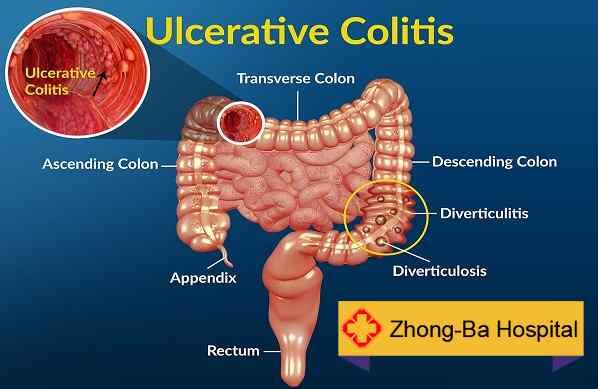
Ulcerative colitis is a medical condition that causes ulcers in the large colon and rectum. It is an autoimmune disease. This condition affects the innermost lining of the large intestine and rectum. Ulcerative colitis is debilitating and can lead to life-threatening complications. Doctors classify ulcerative colitis according to inflammation location. There are four types: ulcerative proctitis , proctosigmoiditis , left-sided colitis , pancolitis .
Figure 01: Ulcerative Colitis
The symptoms of this medical condition include diarrhea, abdominal pain, rectal pain, rectal bleeding, urge to defecate, inability to defecate, weight loss, fatigue, fever, and in children, failure to grow. The risk factors include age , ethnicity , and family history . Moreover, this inflammatory condition can be diagnosed through endoscopy, tissue biopsy, blood test, imaging tests , and stool tests. The treatments include anti-inflammatory drugs , immunosuppressant , biologics targeting immune system proteins , and surgery .
You May Like: Can Foot Ulcers Be Cured
What Is The Difference Between Ulcerative Colitis And Piles
January 11, 2022 Posted by Dr.Samanthi
The key differencebetween ulcerative colitis and piles is that ulcerative colitis is a medical condition that causes ulcers in the large colon and rectum, while piles are a medical condition that causes swollen veins in the anus and lower rectum.
Anal pain is the pain that occurs around the anus and rectum. Often, this pain accompanies bleeding. It is a common symptom of many different medical conditions. Most of the symptoms are minor and go away with treatment. In rare cases, it is a symptom of a serious condition such as anal cancer. Many different medical conditions can cause anal pain, such as ulcerative colitis, piles, anal fissure, anal fistula, anal abscess, infections, etc. Ulcerative colitis and piles are two different medical conditions that are responsible for anal pain.
Also Check: What Is The Best Home Treatment For Hemorrhoids
Rectal Bleeding And Inflammatory Bowel Disease
One of the many symptoms of inflammatory bowel disease is bleeding. Blood might appear in or on the stool or some people may pass no stool at all at times, and just pass blood.
Bleeding from the rectum and large intestine from IBD is typically red or bright red, while blood coming from higher up in the digestive tract could appear as darker or black stools. In most cases this bleeding is slow and steady.
However, you should get emergency attention if:
- Bleeding is severe
- Youre vomiting blood
- You faint or feel like youre going to
Blood in or on the stool can be frightening but it doesnt always mean that theres an emergency. Its sometimes part of an IBD flare-up and it should be discussed with a physician as soon as possible, especially if it hasnt happened in a while.
Bleeding means that there is some inflammation somewhere, and a change in treatment might be needed. Many treatments are available for IBD that can help stop the inflammation and the bleeding.
Also Check: Can You Eat Oatmeal With Ulcerative Colitis
Number 4 Use Supplements If Necessary
As per the introduction earlier, supplements should not be your only strategy.
You should work out what is triggering you, and remove it.
However, some of the following supplements can be useful.
Ive included links in each section to the specific supplements that I generally recommend.
Note the doses Ive recommended are for these specific supplements only.
- Vitamin D low levels of Vitamin D will pose issues for achieving a well-functioning immune system.
Recommended dose: 5,000-10,000 IUs daily, unless your blood work has shown your Vitamin D levels to be adequate.
- Bentonite Clay can help slow down intestinal motility, and bind toxins and bacteria to help you have a well formed poop.
Recommended dose: over the course of 1 week, work up to 2 tbsp daily, taken in 1 tbsp serving sizes in 12oz of water.
Take at separate times of the day away from meals.
Do not take 2 tbsp daily for more than 2 weeks.
- Probiotics / Fermented Foods can help crowd out bad bacteria and other pathogens and help to restore microbial balance in your gut.
Note for people with inflamed guts, Ive occasionally seen probiotics and fermented foods being troublesome.
This is likely due either to the acidity or to an intense Herxheimer reaction, which is why I recommend starting slow.
Probiotics recommended dose: up to 8 capsules daily, taken with or without food.
Start with 2 capsules and work your way up gradually to 8 capsules over the course of several weeks or until your symptoms improve.
Recommended Reading: How Do You Shrink Hemorrhoids
How Hemorrhoids Are Treated
Most external hemorrhoids can be treated with home treatments, such as:
- Adding fiber to your diet, including fruits, vegetables, and whole grains
- Drinking more water
- Avoiding straining during bowel movements or sitting on the toilet for long periods
- Over-the-counter pain relievers such as acetaminophen, ibuprofen, naproxen, or aspirin
- Sitting in a tub of warm water a sitz bath several times a day
Home treatments can also be used for most internal hemorrhoids. But severe internal hemorrhoids may require other treatments.
You should call your doctor if you:
- Still have symptoms after one week of at-home treatment, or
- Have bleeding from your rectum
When home treatments dont heal internal hemorrhoids, your doctor may recommend one of the following treatments performed by a physician:
- Rubber band ligation. This involves placing a special rubber band around the base of a bleeding or prolapsing hemorrhoid. This cuts off the blood supply, causing the hemorrhoid to shrivel and fall off.
- Sclerotherapy. A solution is injected into the hemorrhoid causing scar tissue to form, cutting off the blood supply, often shrinking the hemorrhoid.
- Infrared photocoagulation. The heat of infrared light directed at the hemorrhoid causes scar tissue to form. This cuts off the blood supply, often shrinking the hemorrhoid.
- Electrocoagulation. An electric current is directed into an internal hemorrhoid to form scar tissue, cutting off the blood supply, often shrinking the hemorrhoid.
Can Proctitis Be Prevented
People who receive anal sex can avoid getting STD-related proctitis by having their partner use a condom. If anorectal trauma caused proctitis, stopping the activity that triggered inflammation often will stop the inflammation and prevent recurrence.
Other causes of proctitis cannot always be prevented. However, their symptoms can be treated by a doctor.
Also Check: Is Vaporub Good For Hemorrhoids
Consult The Gastroenterologist Regularly:
During your treatment, your gastroenterologist needs to see you for regular checkups and if you have any concerns or need help to manage Ulcerative Colitis flare-up, you should consult the physician. Establish a good relationship with your doctor and be honest about your symptoms and condition as how they are affecting you because this all helps the gastroenterologist to determine an appropriate treatment plan for you or makes changes in the prescribed treatment plan.
What Are Possible Treatment Options
Anti-inflammatory drugs such as 5-aminosalicylates and corticosteroids are usually recommended during initial efforts to manage UC symptoms. Immune system suppressors like cyclosporine and vedolizumab may also help control the immune system and suppress the process that triggers inflammation.
If ulcerative colitis is causing fevers or infections, antibiotics might be prescribed. Certain pain relievers may be recommended as well. However, ibuprofen and naproxen sodium should be avoided because they may aggravate UC symptoms. Some patients also benefit from:
- Iron supplement to minimize issues with chronic intestinal bleeding
- Anti-diarrheal medication
- A high-protein, high-calorie eating plans that’s also low in fiber
Don’t Miss: How Do You Develop Hemorrhoids
What Is Rectal Bleeding
Although its alarming to find blood in the toilet bowl or on your toilet paper, you probably dont need to worry. Bloody stools should be addressed, but there are many reasons for rectal bleeding that dont warrant an emergency visit to the doctor.
Rectal bleeding is a blanket term that healthcare providers use to talk about any blood that leaves your body from your rectum. This doesnt mean that your rectum is the source of your bleeding the blood could be coming from anywhere in your gut. Another term for this condition is gastrointestinal tract bleeding.
Burning Pain In Your Abdomen

This may seem like a no-brainer but the most common sign that people experience when they have a stomach ulcer is a persistent burning pain in their abdomen. This sensation occurs when juices in the stomach used for digestion come into contact with the open sore. For the most part, the pain is felt from the breastbone to navel and is often worse at night than during the day. On the other hand, if you are someone who frequently skips meals, you may find that you experience this pain much throughout the daytime.
Recommended Reading: Are Eggs Bad For Ulcerative Colitis
Also Check: Why Do I Have Hemorrhoids