What Are The Symptoms
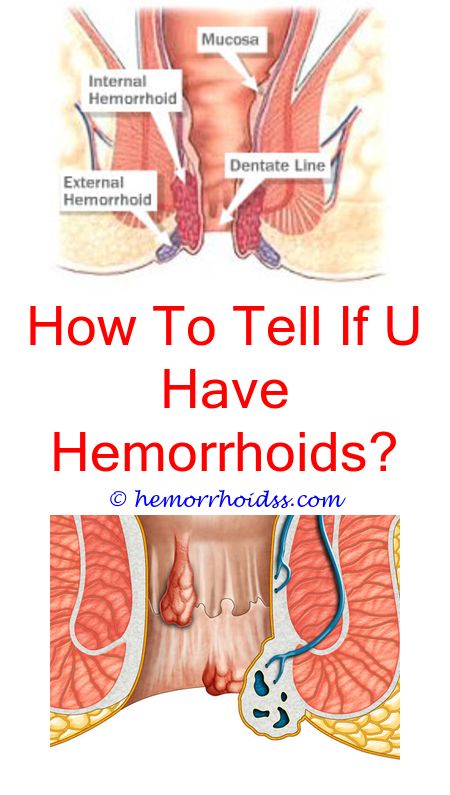
The most common symptoms of both internal and external hemorrhoids include:
- Bleeding during bowel movements. You might see streaks of bright red blood on toilet paper after you strain to have a bowel movement.
- Itching.
- Rectal pain. It may be painful to clean the anal area.
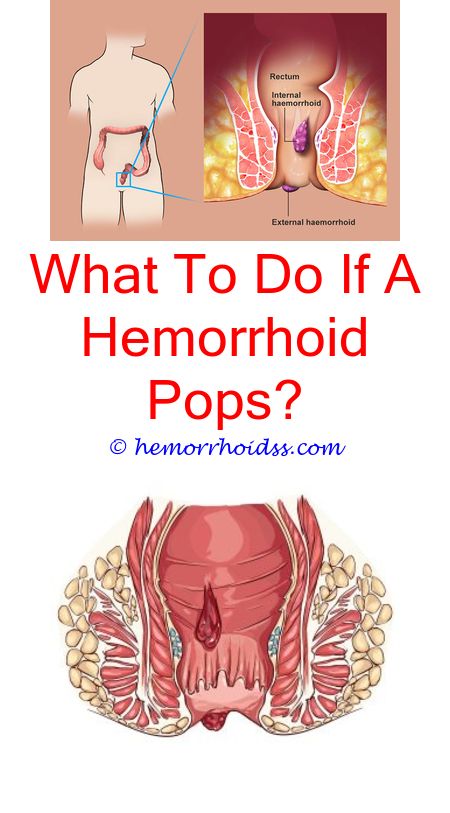
Internal hemorrhoids
With internal hemorrhoids, you may see bright red streaks of blood on toilet paper or bright red blood in the toilet bowl after you have a normal bowel movement. You may see blood on the surface of the stool.
Internal hemorrhoids often are small, swollen veins in the wall of the anal canal. But they can be large, sagging veins that bulge out of the anus all the time. They can be painful if they bulge out and are squeezed by the anal muscles. They may be very painful if the blood supply to the hemorrhoid is cut off. If hemorrhoids bulge out, you also may see mucus on the toilet paper or stool.
External hemorrhoids
External hemorrhoids can get irritated and clot under the skin, causing a hard painful lump. This is called a thrombosed, or clotted, hemorrhoid.
Is Surgery Necessary For External Hemorrhoids
Less than 10 percent of people with hemorrhoids will need surgery. You may need surgery if your hemorrhoid is very large or if you have both external and internal hemorrhoids. Types of surgery for hemorrhoids include: Rubber band ligation: The doctor places a small elastic band at the base of the hemorrhoid.
Learn About Hemorrhoid Surgery & Your Alternative Options
In some cases, your doctor may recommend hemorrhoid surgery, known as hemorrhoidectomy, to remove hemorrhoids. If your doctor has recommended surgery for your hemorrhoids, it is a good idea to learn all that you can about the procedure ahead of time, so you can be comfortable and clear on what to expect.
Typically, hemorrhoid surgery is only needed for the most severe cases. In the vast majority of cases, a less invasive hemorrhoid treatment, such as rubber band ligation, can be just as effective for symptomatic hemorrhoids, without the pain and recovery time.
However, if surgery for hemorrhoids is needed, several types of hemorrhoidectomies are available, and most can be performed on an outpatient basis.
Recommended Reading: What Can I Do For Bleeding Hemorrhoids
Why Is Haemorrhoidectomy Performed
Most haemorrhoids can either be treated with medicines or non-surgical procedures or avoided with appropriate diet and exercise.
If non-surgical treatments don’t work, or the haemorrhoids are particularly large, a doctor might suggest a haemorrhoidectomy.
Removing the haemorrhoids will relieve the uncomfortable symptoms, but haemorrhoids can also return.
Postoperative Care After Hemorrhoidectomy

Most hemorrhoidal flare-ups stop hurting within two weeks without treatment. Eating a high-fiber diet and drinking 8 to 10 glasses of water per day can usually help you manage the symptoms by promoting softer and more regular bowel movements.
You may also need to use stool softeners to reduce straining during bowel movements, as straining makes the hemorrhoids worse. Your doctor may recommend over-the-counter topical ointments to ease occasional itching, pain, or swelling.
Recommended Reading: What Does It Mean When Your Hemorrhoids Bleed
When Is Hemorrhoid Surgery Necessary
Hemorrhoid surgery may be necessary for internal hemorrhoids that have prolapsed if this prolapse is significant, such as when the protruding tissue cannot be pushed back in. If your hemorrhoids are painful, bleeding, or long-lasting, or youre experiencing anal leakage, you should check with your physician to see if you require a hemorrhoidectomy to treat your hemorrhoid symptoms.
Other Treatments Are Just as Effective as Hemorrhoid Surgery
Surgery is not the preferred option to treat most hemorrhoids, as patients may experience postoperative pain, bleeding, or incontinence. There are other hemorrhoid treatments, such as rubber band ligation, that offer relief through less-invasive measures.
The CRH ORegan System is fast and painless, and in most cases provides a permanent solution. The treatment technology involves placing a band around the base of the affected area to cut off the blood supply to the hemorrhoid, causing it to shrink and fall off within a few days. The painless treatment takes thirty seconds to a minute requires no preparation or surgical sedation NPO orders and less than 1% of patients experience post-procedure complications. Hemorrhoid surgery is frequently a last resort, but with the CRH ORegan System, 99% of patients find relief from their hemorrhoid symptoms without surgery.
Hemorrhoids usually dont go away on their own, and to avoid unnecessary, prolonged discomfort, check with your physician to find the right treatment for your situation.
What Causes Internal And External Hemorrhoids And Simple Ways To Treat Them
Hemorrhoids are usually caused by increased pressure due to pregnancy, being overweight, or straining during bowel movements. By midlife, hemorrhoids often become an ongoing complaint. By age 50, about half the population has experienced one or more of the classic symptoms, which include rectal pain, itching, bleeding, and possibly prolapse . Although hemorrhoids are rarely dangerous, they can be a recurrent and painful intrusion. Fortunately, there’s a lot we can do about hemorrhoids.
Also Check: How Do You Know You Have Hemorrhoids
Things That Increase Your Risk
- Constipation or diarrhea that does not go away. These conditions may lead to straining with bowel movements.
- Being overweight
- A family history of hemorrhoids. You may inherit the tendency to get them.
- Being age 50 or older. Half of people who are older than 50 seek treatment for hemorrhoids.
- Pregnancy and labour and delivery. As the fetus grows during the last 6 months of pregnancy, blood volume and pressure on pelvic blood vessels increase. The strain of labour also can cause hemorrhoids to start or get worse.
- Liver disease, heart disease, or both. These conditions may cause blood to back up in the pelvis and abdomen.
Complications Of A Rubber Band Ligation Of Hemorrhoids
This outpatient hemorrhoid treatment is another method of ridding your body of internal hemorrhoids. Rubber band ligation works to stop the flow of blood to the hemorrhoid that is irritated, and the mass will shrink and die within a few day of the bands’s application.
Complications that are possible after a rubber band ligation surgery are:
- Infection
- Thrombosed hemorrhoids
- Ulcers
Hemorrhoid bleeding and pain are relatively common post ligation surgery, but if you have had this procedure done and found that the site is possibly infected, or there are a presence of ulcers, thrombosed hemorrhoids, and excessive and persistent bleeding, contact your physician immediately.
These complications, although rare, should be taken seriously.
Hemorrhoids are enough of a pain and any complications that may arise should be immediately relayed to a doctor.
Complications that result from cases of hemorrhoids can be rare. Fortunately, for a healthy, normal body, the healing time is relatively fast.
Hemorrhoids are reported to only hang around for a few days and up to a few weeks at most.
Inflamed hemorrhoids shrink, and can shrink faster with proven and effective treatment methods.
Anything to calm the skin that can be applied to external hemorrhoids will help make them shrink faster, whereas, with internal hemorrhoids, a diet of increased fiber will do the trick in keeping your inner rectal lining in its normal condition.
Also Check: Can You Have Hemorrhoids And Not Know It
When Should You Get Hemorrhoid Surgery
Your healthcare provider may suggest surgery if you have large hemorrhoids, both internal and external hemorrhoids, or bleeding and pain that isn’t managed with other non-surgical treatments. With small hemorrhoids, your healthcare provider will usually suggest lifestyle changes first, such as eating a high-fiber diet and drinking lots of water.
What To Expect After A Haemorrhoidectomy
After the surgery, you’ll probably be in quite a bit of pain especially when opening your bowels and you might have some bleeding.
Many people go home the same day, but make sure you are collected by someone who can take you home.
You should follow any directions you are given by your clinic. For example, you may be asked to take stool softeners for some time to reduce discomfort in emptying your bowels when you use the toilet
It is important to avoid constipation, so you should drink plenty of water and eat a healthy diet that is high in fibre, fruit and vegetables.
The general anaesthetic might make you feel sick and tired for a few days. Many people need to take 1to 2 weeks off work to recover.
Your doctor will probably ask you to return for a check-up sometime after your operation.
Don’t Miss: How To Get Rid Of Hemorrhoids Naturally
Simple Painless Hemorrhoid Treatment Without Surgery
Sign Up for Our Free E-Newsletter
Receive updates delivered straight to your inbox about new services and upcoming events.
Hemorrhoids are a common cause of discomfort, affecting 75 percent of people within their lifetime. They can also be uncomfortable to talk about, and many people seek the temporary relief provided by ointments and creams in the hope their hemorrhoids will simply go away so they can avoid the prospect of painful surgery. Now, Capital Health offers patients another option: hemorrhoid banding with the CRH ORegan System.
The CRH ORegan System is a non-surgical treatment option for hemorrhoids that is fast, painless, and proven to be effective, with minimal risk of complications, said Dr. Michael Kalina, board certified general surgeon at Capital Health Surgical Group. With no preparation or sedation required, the procedure can be performed in as little as 60 seconds. Patients can drive themselves to and from the appointment and immediately return to their daily lives.
Banding is the most common non-surgical hemorrhoid removal treatment in use today. A rubber band is placed around the base of the symptomatic hemorrhoid to stop blood flow to the tissue, which then dries up and falls off on its own in a week or two . Where conventional banding equipment uses metal-toothed forceps to grasp the hemorrhoid, the CRH ORegan System uses gentle suction to reduce the risk of pain and bleeding.
What Can Go Wrong
Haemorrhoidectomy is a common and generally safe surgical procedure. But there can also be complications, including:
- excessive bleeding
- infection, which might cause a high temperature
- loss of control of the rectal sphincter
- narrowing or damage to the anal canal
If you have any of these symptoms, or the pain around your anus gets worse rather than better, you should call your doctor for advice.
Read Also: What Is The Remedy For Hemorrhoids
Care After Hemorrhoid Surgery
Pain is the most common complaint, especially when youre pooping. You can take over-the-counter pain relievers, such as acetaminophen, aspirin, or ibuprofen, if your doctor says its OK. Soaking in a warm bath may help, too.
Stool softeners can make it easier to poop.
Risks
Its very common and is considered safe. However, any surgery has some risks including:
- Bleeding
- Reaction to anesthesia
You might have some trouble peeing afterward because of swelling or muscle spasms.
If your anal sphincter gets damaged during surgery, you could have accidental bowel or gas leaks, a condition called fecal incontinence.
Purpose Of Hemorrhoid Surgery
The purpose of hemorrhoid surgery is to remove external or internal hemorrhoids.
That said, even though hemorrhoidectomy is the most effective and definitive treatment for hemorrhoids, it’s linked to significantly more pain and complications than non-surgical therapies.
Therefore, the American Gastroenterological Association advises that surgery only be considered for a specific and small group of individuals.
Potential candidates for hemorrhoidectomy generally include patients who:
- Have tried medical and non-operative hemorrhoid therapies without success, or who cannot tolerate them
- Have grade 3, grade 4, or mixed internal and external hemorrhoids that cause symptoms
- Have symptomatic hemorrhoids along with an associated anorectal condition that warrants surgery
- Prefer surgery and have discussed therapy options with their referring healthcare provider and surgeon
When hemorrhoid surgery is scheduled, various pre-operative tests may need to be run, especially for patients undergoing general anesthesia.
Examples of such tests include:
Recommended Reading: What Doctor Do You See About Hemorrhoids
Can Hemorrhoids Be Treated Without Surgery
A very common question that I am asked is whether everyone with hemorrhoids needs surgery. And the truth of the matter is that only a minority of patients need surgery for hemorrhoids. Many times, I am actually able to treat hemorrhoids more effectively in the office than in the operating room. So, who can be treated in the office and who needs surgery for hemorrhoids?
First, we should talk about the difference between external and internal hemorrhoids. Ive talked about this difference in another post as well. External hemorrhoids have pain nerves and cant be treated with hemorrhoid banding. Imagine if you put a rubber band on your finger it would hurt thats why you cant rubber band external hemorrhoids. But, internal hemorrhoids dont have pain nerves. They have nerves known as autonomic nerves, which supply sensations similar to the intestinal tract . Because internal hemorrhoids dont have pain nerves, they can be treated with procedures in the office.
Theres a grading scale for hemorrhoids. Its useful to understand this so we can talk about different types of hemorrhoids:
* First Degree Bleed only, but do not prolapse
* Second Degree Bleed, prolapse, but spontaneously reduce
* Third Degree Bleed, prolapse, and require manual reduction
* Fourth Degree Bleed, prolapse, and are irreducible
Thanks for joining!
Why You Probably Dont Need Hemorrhoid Surgery
Hemorrhoids are cushions of swollen tissue and blood vessels in your lower rectal region. They manifest in two ways, each with different symptoms: internal hemorrhoids form inside your rectum where there arent any pain-sensing nerve endings, so unless you experience rectal bleeding, you may not even be aware of them. External hemorrhoids present as bulges or bumps around the anus and are often the cause of the discomfort people associate with hemorrhoids. Its possible to have both internal and external hemorrhoids at the same time.
While nearly 75% of all Americans will have hemorrhoids at some point in their lives 50% will have experience them before they turn 50 only the most severe cases require surgery to have them removed.
Also Check: How To Help Bleeding Hemorrhoids
Stapled Hemorrhoidectomy For Prolapsing Hemorrhoids
Stapled hemorrhoidectomy is the newest addition to the armamentarium of surgical internal hemorrhoid procedures. It has several aliases, including Longo’s procedure, the procedure for prolapse and hemorrhoids , stapled circumferential mucosectomy, and circular stapler hemorrhoidopexy.
Stapled hemorrhoidectomy is mostly used in patients with grade III and IV hemorrhoids and those who fail prior minimally invasive treatments. During stapled hemorrhoidectomy, a circular stapling device is used to excise a circumferential ring of excess hemorrhoid tissue, thereby lifting hemorrhoids back to their normal position within the anal canal.
Stapling also disrupts hemorrhoid blood supply. Studies have suggested that stapled hemorrhoidectomy results in less postoperative pain and shorter recovery compared with conventional surgery, but a higher rate of recurrence. Frequency of complications is similar to that following standard hemorrhoidectomy.
Stapled Hemorrhoidectomy
Source: Hemorrhoids:By Andrea C. Bafford, M.D. and Ronald Bleday, M.D . Version 20. Knol. 2008 Jul 28 , Creative Commons Attribution 3.0 License
How Do I Prepare For A Haemorrhoidectomy
If you are having a haemorrhoidectomy, you should follow the guidelines your hospital or clinic gives you on how to prepare for the procedure.
You will be asked not to eat or drink some hours before admission to the clinic. If you usually take blood-thinning medication, you might be asked to stop taking it some days before the procedure.
You might also be asked to take an enema or laxative to empty out your bowel.
Learn more about how to prepare for surgery here.
Recommended Reading: How To Get Rid Of Large External Hemorrhoids
How Are They Treated
For most external hemorrhoids, home treatment is all you need. This includes slowly adding fibre to your meals, drinking more water, and using over-the-counter ointments for a limited time to stop itching. You also may use stool softeners. The same home treatment can be used for most internal hemorrhoids.
If your internal hemorrhoids are severe, you may need other treatment. The doctor may tie off the hemorrhoids with rubber bands or scar the tissue around the hemorrhoids. These treatments reduce the blood supply to the hemorrhoids so that they shrink or go away.
Surgery to remove hemorrhoids may be done if other treatments don’t work.
Healthy habits can help you prevent hemorrhoids or keep them from getting worse. Eat foods that have lots of fibre, such as fruits, vegetables, and whole grains. Also, drink plenty of water, and get plenty of exercise.
Hemorrhoidectomy Versus Fixative Procedures For Internal Hemorrhoids
- Fixative procedures are usually tried before surgery if hemorrhoids are small and stick out of the anus during a bowel movement but return to their normal position afterward .
- Hemorrhoidectomy may provide better long-term results than fixative procedures. But surgery requires a longer recovery time, is usually more painful, and has a greater risk of complications.
- Fixative procedures are the preferred treatment for people older than age 70 and for people in poor health.
You can help prevent the irritating and painful symptoms of hemorrhoids.
Read Also: Does Urgent Care Treat Hemorrhoids
Diagnosing And Classifying Hemorrhoids
Hemorrhoids are the distal prolapse of the arteriovenous bundle, muscle fibers and surrounding connective tissue as an envelope below the dentate line in the anal canal. They usually present with painless rectal bleeding.2
The diagnosis of hemorrhoids relies on history and physical examination rather than on laboratory testing or imaging studies. Typically, the presenting symptom is painless rectal bleeding associated with bowel movements, usually appearing as bright red blood on the toilet paper or coating the stool. Severe itching and anal discomfort also are common, especially with chronic hemorrhoids.
Complications Of A Hemorrhoidectomy
A hemorrhoidectomy is a surgery aimed at hemorrhoid removal. This surgery is for those with severe and enlarged hemorrhoids with the risk of rupturing, causing further complications.
It is imperative to keep a close eye on your body post-operation, especially the first ten or so days.
Complications that can occur after a hemorrhoidectomy surgery are:
- Anal fissures, tears in the anal lining
- Fever
- Problems and difficulty urinating or defecating
- Excessive swelling in the anal area
- Constipation
These complications can be rare, but if you are experiencing any of them, inform your hemorrhoid doctor because you may require hospitalization.
Don’t be afraid of trying a new product for hemorrhoids that works. HemRid is an outstanding product for hemorrhoids that works great.
Also Check: What Cream To Put On Hemorrhoids