Are Hemorrhoids Good Or Are They Bad
Both. As they cushion the anal opening during a bowel movement, they also can enlarge and cause many symptoms. Nobody knows exactly why hemorrhoids become symptomatic. Too much pushing during a bowel movement? Pregnancy? Obesity? Hereditary? There are as many possible reasons for hemorrhoids enlarging as there are symptoms. Symptoms include:
- Bleeding
- Discharge
Suction Vs Forceps Ligation
A prospective randomized clinical trial including 100 patients with second- and third-degree hemorrhoids compared suction and forceps ligation concerning pain after the procedure, intra-procedure bleeding and other complications. The forceps group had higher pain scores immediately after ligation and at 24 h post-banding, needed higher amount of analgesia and had higher intra-procedure bleeding. Authors hypothesized that this is due to poorer visualization and forceps-induced physical trauma of the friable hemorrhoids.
The History Of Hemorrhoid Banding
Humans have been treating hemorrhoids for thousands of years. Before the invention of rubber band ligation, physicians used a range of methods to relieve hemorrhoid symptoms, including various surgical and ligation techniques. For example, during the fifth century B.C., Hippocrates wrote about a procedure similar to rubber band ligation, which involved tying hemorrhoids with a thick woolen thread until they drop off.
It wasnt until the 1950s that Paul C. Blaisdell first described rubber band ligation as we know it today. The procedure was based on Blaisdells idea that internal hemorrhoids are easy to access and have few pain-sensitive nerve endings. Due to the procedures simplicity, doctors could use rubber band ligation to provide hemorrhoid treatment in their office rather than in a hospital.
Then, in the 1960s, J. Barron modified outpatient hemorrhoid ligation by using rubber bands and a device called the Barron band ligator. The Barron hemorrhoid ligator is a metal device that uses forceps to grasp the hemorrhoid before placing a rubber band around its base. Since Barrons technique, various types of forceps have been invented to perform rubber band ligation.
Even though Barrons ligation method is generally considered simple and safe, it needed improvement. Doctors found that grasping the hemorrhoid with forceps wasnt always easy and could cause post-procedure pain.
Today, over a million rubber band ligations have been performed using CRH ORegan technology.
You May Like: How To Tell The Difference Between Hemorrhoids And Cancer
Nursing Allied Health And Interprofessional Team Interventions
Patients should maintain stool soft with hydration, fiber use, and stool softener. Minor discomfort should be managed with acetaminophen. Office staff also help to ensure the patient has given written consent as well as educating the patient about the treatment of hemorrhoids. Nursing staff help position the patient and assist with the procedure.
How Many Times Can The Same Hemorrhoid Be Banded
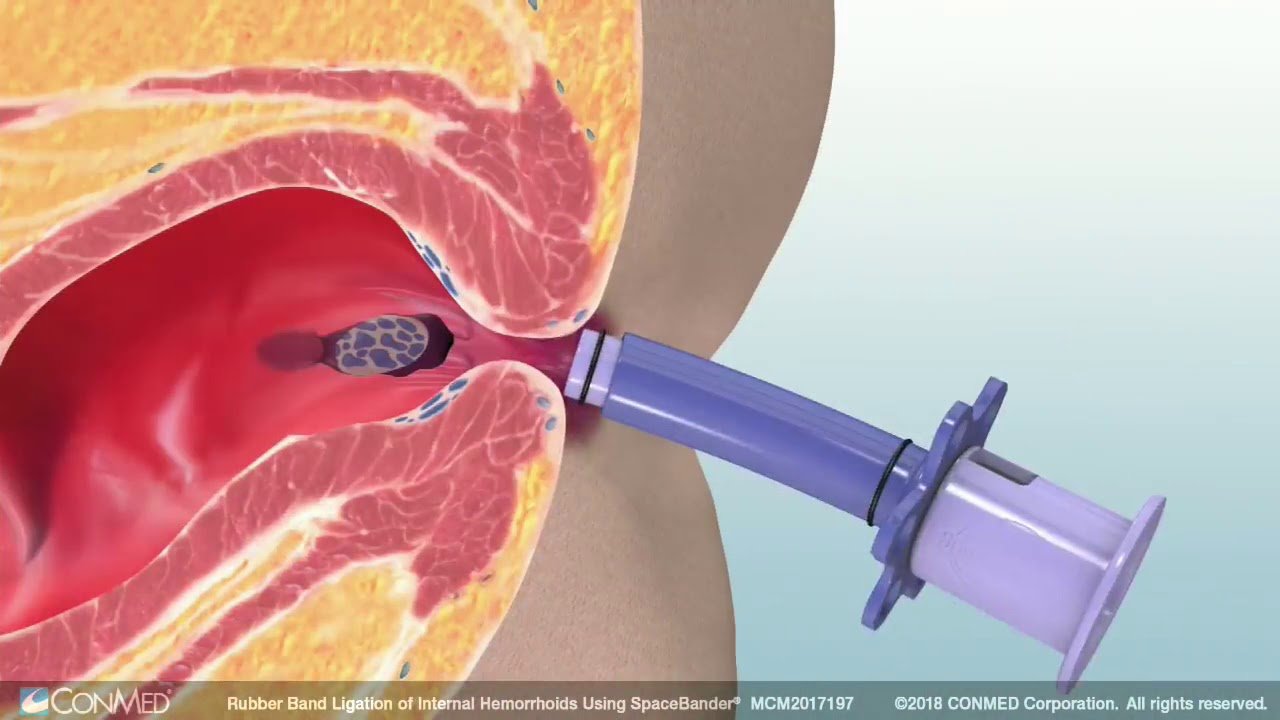
You may require up to three sessions at two week intervals as all people have 3 hemorrhoidal veins. Only one hemorrhoid is ligated during each session to minimize complications and discomfort.
How many times can you have hemorrhoids banded?
Your physician will likely only place one band per session, as treating multiple hemorrhoids simultaneously may increase the risk of pain, discomfort or various complications. Hemorrhoids typically form in three sites, meaning most patients need three treatments for maximum effectiveness.
How is a hemorrhoid removed with rubber band ligation?
To remove a hemorrhoid using rubber band ligation, your doctor inserts a small tool called a ligator through a lighted tube in the anal canal and grasps the hemorrhoid with forceps. Sliding the ligators cylinder upward releases rubber bands around the base of the hemorrhoid.
How is infrared coagulation used to treat hemorrhoids?
Infrared Coagulation In this office-based procedure, the doctor uses an intense beam of infrared light to shrink the hemorrhoid. Heat from the light causes the formation of scar tissue, cutting off the blood supply to the hemorrhoid.
You May Like: What Foods To Avoid With Hemorrhoids
The Benefits Of Hemorrhoid Banding
Hemorrhoid banding is an effective procedure where a band is placed at the base of an internal hemorrhoid to reduce the overall blood flow to the pile. In most cases, a hemorrhoid requires multiple banding sessions to be treated effectively. Within a few days of your final hemorrhoid banding treatment, the pile will naturally and painlessly fall off, typically during a bowel movement.
Some of the main benefits of hemorrhoid band ligation include:
Can I Rubber Band Hemorrhoids At Home
No, only a trained and licensed medical professional should do a rubber band procedure.
Banding procedures are used on internal hemorrhoids, which are not visible or exposed.
This procedure requires a doctor to insert a ligator, which will pull and suction away the hemorrhoid in order to place the band on the base.
While you cannot rubber band hemorrhoids at home, you can make your recovery time from the procedure more comfortable by taking warm baths, soaking your lower and rectal region for about 20 to 30 minutes.
Sitz baths are also helpful tools that fit over the bowl of a toilet, allowing you to soak just the lower area.
Rubber banding hemorrhoids is an effective method for solving a persistent hemorrhoid issue.
It is recommended to those suffering from constant hemorrhoids and when natural or medicinal treatments are not helping with symptoms or in prevention.
This procedure is proven to be both safe and effective.
Complications that arise post procedure should be immediately recognized and reported to your doctor
Recommended Reading: What Causes Hemorrhoids In Pregnancy
Enhancing Healthcare Team Outcomes
Hemorrhoidal disease can sometimes be difficult to distinguish from other anorectal pathologies and, as such, may be treated incorrectly. The disorder is best addressed by an interprofessional team dedicated to anorectal conditions.
All members of the interprofessional team evaluate patients with hemorrhoids in different settings, such as the office, emergency department, or urgent care. An understanding of the degree of prolapse of internal hemorrhoids is essential and helps the healthcare professional choose the adequate treatment, the need for referral to a colorectal specialist, and provide an appropriate education. Correct diagnosis of an acutely prolapsed incarcerated internal hemorrhoid leads to proper treatment promptly, which increases overall patient safety and satisfaction.
Several vital clinical recommendations are published for practice:
The primary care physician, nurse, and pharmacist should encourage the patient to avoid constipation, drink ample water, be physically active, add fiber to their diet, and refrain from using narcotic pain medication. Interprofessional team management involving clinicians, nursing, and pharmacy can drive better patient outcomes.
Hemorrhoid Banding Cpt Code: A Quick Guide
If youre planning to add hemorrhoid banding as a service offered by your medical facility, then youre going to need to learn the appropriate codes related to this procedure. Knowing the correct Current Procedural Terminology codes can reduce confusion and streamline your offices billing practices.
To get started, review the following hemorrhoid banding CPT code guide. It will walk you and your office staff through the ins and outs of coding and reimbursement for treatment with a hemorrhoid banding ligator.
Read Also: How To Get Hemorrhoids To Go Away
Hemorrhoids Rubber Band Ligation
Hemorrhoids rubber band ligation is a very common treatment to painlessly eliminate hemorrhoids in an outpatient clinic. This modality of treatment is generally called instrumental treatment of hemorrhoids.To understand what the indications for instrumental treatment are, one must have in mind the classification of hemorrhoids.
GRADES are a simple conventional system of classifying hemorrhoids: 1st degree: small hemorrhoids, which never prolapse 2nd degree: haemorrhoids that prolapse, but which spontaneously shrink 3rd degree: haemorrhoids that prolapse and that the patient must manually reduce 4th degree: hemorrhoids that can no longer be reduced.
When To Talk To A Doctor About Hemorrhoids
In general, it is always a good idea to talk to your physician about hemorrhoidal symptoms, even if they are not severe. If you are looking for a hemorrhoid doctor in your area, you can use CRH ORegans clinic locator to find a specialized physician, trained in hemorrhoid banding. Early treatment can help minimize the risk of hemorrhoids worsening or advancing grades.
If you notice intense pain or severe symptoms, like excessive bleeding or intense itchiness that disrupts daily life, you should contact your doctor as soon as possible. Your physician can address these symptoms and ensure there are no other diseases or complications that may be causing them. Talking with your physician can also help you create an effective treatment plan customized for your unique needs.
Hemorrhoid banding is often recommended for patients who experience prolapsed hemorrhoids that cause itching, soiling, bleeding or swelling. The banding procedure is an effective treatment that can alleviate symptoms for most patients. Still, it is important to note not all techniques are the same or provide the same results.
Talking with your physician can help you learn more about hemorrhoid banding and the various techniques and procedures available. It can be helpful to ask your doctor if they offer hemorrhoid banding using the CRH ORegan System, which is generally viewed as the most effective treatment currently available.
You May Like: What Is The Purpose Of Hemorrhoids
Is Hemorrhoid Banding Considered Surgery
No, hemorrhoid banding is not considered surgery because it does not involve sedation or incisions. Hemorrhoid banding is a nonsurgical internal hemorrhoid treatment.
While hemorrhoid banding is incredibly effective, traditional surgery may be necessary for some patients if symptoms do not improve after three or four treatments.
Recurrence Rate Within 1 Year
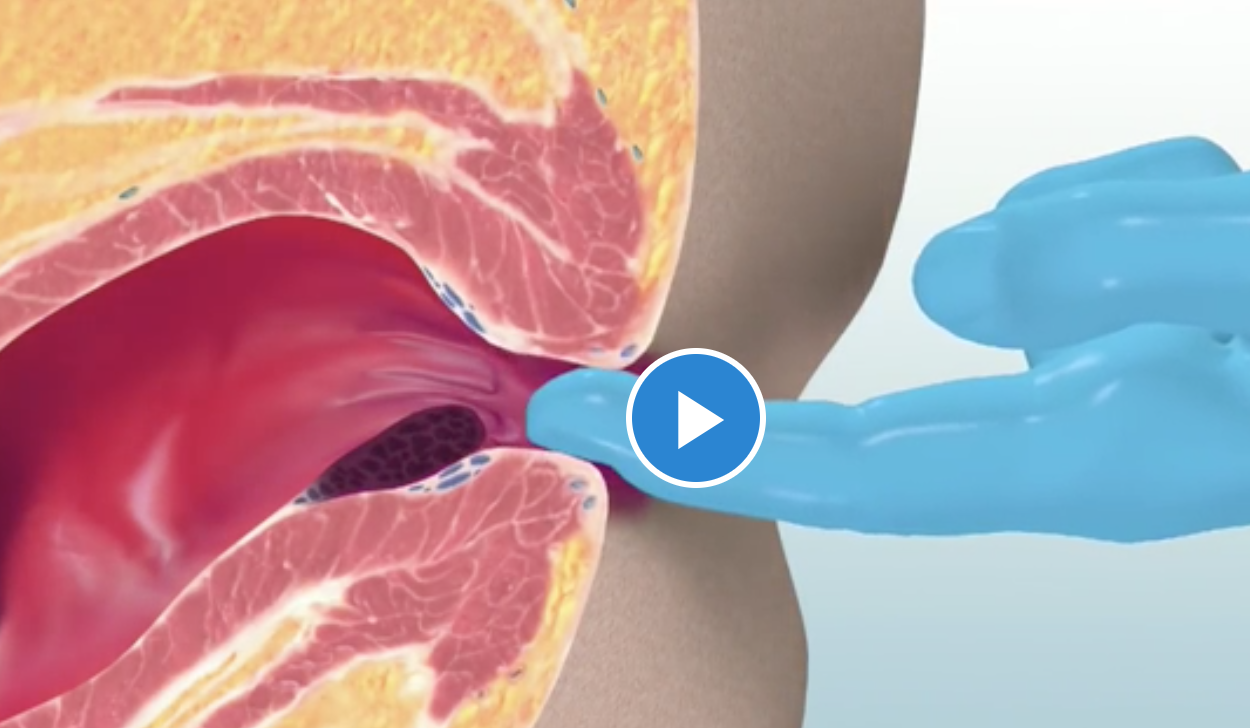
None was lost to follow up in two groups, and serious adverse effects were not observed in two groups. In the MRBL group, 1 patient developed bloody stool , and 3 patients developed prolapsing hemorrhoid which could be reduced spontaneously. In the MMH group, 2 patients developed blood stool . The accumulated recurrence rate was similar between two groups .
Figure 3
Recommended Reading: How To Heal Painful Hemorrhoids
Banding Hemorrhoids Recovery Time
The recovery time for this rubber banding ligation is about 2 to 3 days in order to return to normal activities.
Following your rubber band procedure, your doctor will usually recommend bed rest for these first few days.
Recovery time can go more smoothly and quickly if you do not engage in any strenuous activities.
It is important to continue to rest, even if you think you have fully recovered.
Here are the side effects associated with Rubber Band Ligation:
If you have any of these side effects you should let your hemorrhoid doctor know right away.
Avoid any strenuous exercising that can put any additional stress on your lower rectal region like riding bikes, weightlifting of any degree, and even jogging.
Only resume exercising when your doctor gives you approval.
Walking is encouraged because this will increase circulation and help with your recovery.
A fast-paced walk each day for about 15 to 30 minutes will help increase blood flow but not overwhelm and strain the body.
Avoid heavy lifting, as this could prolong your recovery, produce excess bleeding, and cause further, unnecessary harm.
Heavy lifting can include what you may consider menial, like groceries, small boxes, or heavy bags.
You should avoid heavy lifting for about 2 to 3 weeks.
Additional Cpt Codes To Know
There are a few other CPT codes that can be used for hemorrhoid banding in some cases. The main situation in which you might need a different code is when ligation is performed with a flexible scope instead of a rigid one.
For example, when hemorrhoid banding is performed during a colonoscopy, you should put down code 45298. The description for that code is Colonoscopy, flexible with band ligation .” If the accompanying procedure is a sigmoidoscopy, then the code is 45350. Its description is Sigmoidoscopy, flexible with band ligation .
However, if the banding is performed with a rigid scope, you will stick with code 46221. Typically, anoscopy is considered part of the banding service and not a separate charge. Billing separately for the scope should only be done if it has a distinct purpose, such as diagnosing a different condition.
If you have a situation in which it seems appropriate to list both the scoping and banding procedures, then you should use 46600 for anoscopy or 45300 for proctoscopy. For either one, including modifier 59 is essential.
Recommended Reading: How Long Does It Take To Get Rid Of Hemorrhoids
How Are Hemorrhoids Treated
The pain from hemorrhoids can be very uncomfortable. Your doctor may suggest a combination of several treatments such as a warm bath followed by an ice pack several times a day. Over-the-counter hydrocortisone suppositories or hemorrhoid creams can provide some relief. Your doctor may also recommend a procedure called rubber band ligation.
How Is A Rubber Band Ligation Performed
Before the procedure
- You may have to stop taking blood thinners such as Coumadin and Aggrenox , four-five days before the procedure.
- You may be asked to sign an informed consent form that consists of the risk and benefits, alternatives, expectations, and length of the procedure.
- You may be given an enema on the previous night of the procedure.
- You may have to fast from midnight to the procedure.
During the procedure
- The physician performs a rubber band ligation either in a hospital or an office setting. Anesthesia may not be necessary while performing this procedure in an office setting.
- The physician inserts a small tool, known as a ligator, through a lighted tube in the anal canal and grabs hemorrhoids with forceps.
- The physician pushes the ligators cylinder to release the rubber band around the base of hemorrhoid.
After the procedure
Post-procedure pain is likely for 24-48 hours. Taking Tylenol can ease the pain.
- Bleeding may be observed for 7-10 days post the procedure.
- Avoid strenuous work for 24-48 hours after the procedure.
- Do not lift anything heavy for 24-48 hours.
- Avoid straining while defecating because it can lead to more hemorrhoids.
- Check out for the following symptoms:
Also Check: Do Hemorrhoids Bleed When You Poop
What Causes Hemorrhoids
When the veins near your anus stretch during the pressure of a bowel movement, a hemorrhoid can develop. If you sit for long periods of time on the toilet or have chronic constipation or diarrhea, a hemorrhoid can occur. Pregnancy, sitting or standing for prolonged periods of time, even regular heavy lifting, can all cause hemorrhoids.
As you age, the risk of hemorrhoids increases because the veins in your anus can weaken and stretch over the years.
What Is A Hemorrhoid
Hemorrhoids are swollen veins located in your anus and lower rectum. Hemorrhoids cause a number of symptoms that can alert you to the condition, including:
- Irritation, pain, burning, or discomfort in the anal region
- Itching and swelling around your anus
- Bleeding
The condition can occur inside the rectum or under the skin around the anus itself .
You cant typically see internal hemorrhoids inside the rectum but straining when passing a stool can cause a few symptoms such as bright red blood in the toilet bowl. External hemorrhoids may bleed, itch, or burn. You may also suffer from a thrombosed hemorrhoid that causes a hard lump near your anus with pain and inflammation.
Also Check: What Is The Best Thing To Shrink Hemorrhoids
How Is It Done
Hemorrhoid banding is usually an outpatient procedure, meaning you wont need to stay in a hospital. Your doctor might even be able to do it in their usual office.
Before the procedure, youll be given anesthesia or have a topical anesthetic applied to your rectum. If your hemorrhoids are very painful, or you need to have a lot of them banded, you may need general anesthesia.
Next, your doctor will insert an anoscope into your rectum until it reaches the hemorrhoid. An anoscope is a small tube with a light at the end of it. Theyll then insert a small tool called a ligator through the anoscope.
Your doctor will use the ligator to place one or two rubber bands at the base of the hemorrhoid to constrict blood flow. Theyll repeat this process for any other hemorrhoids.
If your doctor finds any blood clots, theyll remove them during the banding process. In general, hemorrhoid banding only takes a few minutes, but it could take longer if you have multiple hemorrhoids.
When Does A Doctor Recommend Hemorrhoid Banding
Your doctor may recommend rubber band ligation to treat hemorrhoids that are prolapsed or causing symptoms such as:
- Pain
- Swelling
- Soiling
Hemorrhoids can become itchier or more painful over time if they remain untreated. Any patient who suffers from recurring hemorrhoid symptoms might consider hemorrhoid banding.
Don’t Miss: What Can Cause Hemorrhoids To Bleed
Whats The Recovery Like
After the procedure, the hemorrhoids dry up and fall off on their own. This can take between one and two weeks to happen. You may not even notice the hemorrhoids fall out, since they usually pass with bowel movements once theyre dried up.
You may feel some discomfort for a few days after hemorrhoid banding, including:
- gas
How Does Rubber Band Ligation Work
Rubber band ligation is an office procedure. No special preparation is needed. The patient lays comfortably on an exam table. An anoscope is inserted into the rectum to allow for visualization. A special grasper picks up the hemorrhoid, and a pre-loaded rubber band holder slides down the grasper and onto the base of the hemorrhoid. The surgeon then presses a handle which slides the rubber band down over the hemorrhoid. Thats it. The procedure usually takes one minute or less.
Within ten days, the hemorrhoid, deprived of its blood supply, falls off.
Don’t Miss: How To Get Rid Of Recurring Hemorrhoids
How Do Hemorrhoids Form
Very similar to varicose veins in the lower extremities, hemorrhoids are puffy, tender blood vessels located in the anus and rectum. Some hemorrhoids bulge and prolapse from the anus, causing substantial discomfort and itchiness. Gastroenterologists in California and across the country classify hemorrhoids as internal, or hidden inside the rectum, or external, located around the mucous membranes of the anus.
Both kinds of hemorrhoids form due to muscular weakness in the lower GI tract and to repeated pressure on the veins in the anus and rectum. This pressure comes from:
- Pregnancy
- Straining while attempting bowel movements
- Avoiding bowel movements instead of going to the bathroom right away